In February 2021, South Africa rolled out its national COVID-19 vaccination programme as an initiative to curb the pandemic. As the roll-out progressed, the vaccine was made widely available and cost-free to all South Africans, with the expectation that the uptake would be high. Since then, however, a vaccine democracy survey conducted by a consortium from the University of Johannesburg and the Human Sciences Research Council (UJ/HSRC) and its partners has revealed concerning trends and patterns of low vaccine uptake among South Africans.
The survey results released in December 2021 showed that, over the last three of the five rounds of the survey (December 2020 – November 2021), vaccine acceptance rates had grown exponentially. These results were consistent with those from an earlier survey conducted by the HSRC and partners between June and September 2021 – the “One Year Later” survey. The results of the latter showed that just under two thirds (63%) of participants had reported an intention to take the vaccine.
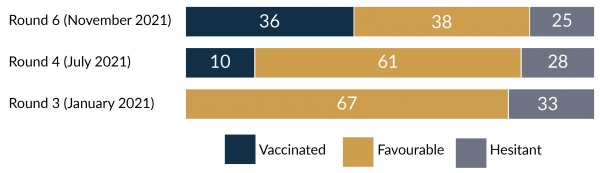
Despite these acceptance rates, the HSRC’s Prof Narnia Bohler-Muller said that only 42% of the adult population had been vaccinated at the time.
What then accounted for the gap between the number of South Africans who felt favourably towards the vaccine and those who had actually been vaccinated? And why, despite a gradual increase in vaccine acceptance, were more than a third of South Africans still hesitant?
Barriers to vaccination
The UJ/HSRC COVID-19 Democracy Survey found that the main barrier to vaccination was concern about perceived short- and longer-term side effects. Concerns about side effects were reported across all age-groups in the adult population (Figure 2).
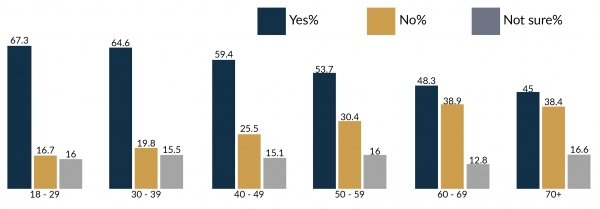
One common fear, according to Dr (Prof) Ramneek Ahluwalia from Higher Health, is the perceived effect on reproductivity and the menstrual cycle. Evidence shows that vaccination does have an impact the menstrual cycle, but the effect is small and temporary – researchers found that each dose was associated with a one-day increase in the current cycle length, on average. Acknowledging side effects and providing accurate information about their magnitude is important for retaining the credibility of public health messaging. Ahluwalia said that many other concerns were not based on scientific evidence but the result of infodemics and misinformation that emanated mostly from social media.
Among vaccine-accepting adults (those who indicated that they would probably or definitely get the vaccine), structural barriers to vaccination uptake were also common. These included not knowing where to get vaccinated, difficulty accessing a vaccination site, cost-related barriers and time constraints. (Figure 3).
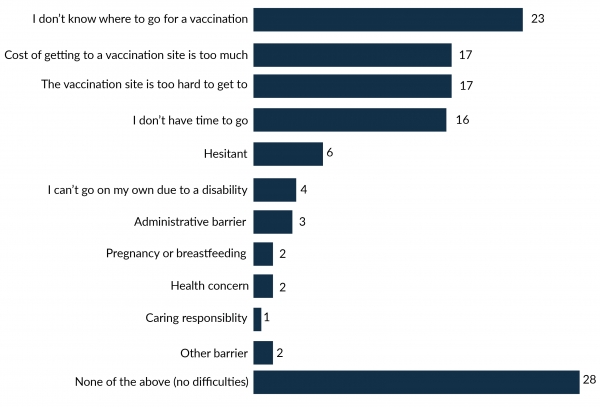
- Multiple response questions asked respondents whether any of six pre-recorded barriers prevented them from getting the COVID-19 vaccine.
- Open-ended ‘other barriers’ responses were also coded and integrated.
- Four reasons predominated among vaccine-favourable adults: not knowing where to get vaccinated (23%), difficulty accessing a vaccination site (17%), cost-related barriers (17%), and time constraints (16%).
- Less-mentioned challenges (6% or less) included general hesitancy, disability, administrative factors, health concerns, pregnancy and caregiving responsibilities.
- 28% mentioned no difficulties in accessing vaccination.
